As some cronistas recorded it, Spaniards on their way to invade Peru reportedly fell ill when they reached the coasts of Ecuador, suffering from high fevers and giant buboes on their bodies. They called the disease verrugas, although its transmission vector remained obscure until the beginning of the twentieth century when the phlebotomine sand fly (Lutzomyia verrucarum) was identified as the culprit.
Diseases are often understood as manifestations of their interaction with mammal species like ourselves, and during the second half of the nineteenth century, physicians also conceived of them as resulting from particular pathological climates around the world. This framing, however, fails to recognize the important role played by nonhuman actors, such as insects that carry disease. By positioning these tiny sandflies as the main driver of the history of Carrión’s disease—as verrugas later came to be known—we can explore how something that Peruvian physicians used to see as a sui generis national pathology can be understood in terms of a more-than-human past.
In 1858, physician Tomás Salazar pioneered the study of the disease and found that most recent cases had originated in the Huarochirí gorges, east of the Peruvian capital. Many Peruvian medical students at that time were interested in analyzing how both “foreign” diseases like yellow fever and “local” ones like verrugas were influenced by domestic environmental factors. This led to extensive research in the following decade, confirming Salazar’s hypothesis that the disease’s etiology was linked to the temperate climate and high humidity in the valleys surrounding the upper course of the Rimac River.

Fig. 1. Zones of verrugas in the Quebradas of Rimac, 1898.
Fig. 1. Zones of verrugas in the Quebradas of Rimac, 1898.
Originally published in Ernesto Odriozola, La Maladie de Carrion, ou la Verruga péruvienne (Paris: G. Carré et C. Naud, 1898). Courtesy of Archive.org.
 This work is licensed under a Creative Commons Public Domain Mark 1.0 License.
This work is licensed under a Creative Commons Public Domain Mark 1.0 License.
During the Guano Age (1845–1879), the disease was further identified with the trans-Andean gorges due to the elite classes’ ambition of introducing industrial capitalism to the Central Highlands. Presidents José Balta and Manuel Pardo aimed to connect the Andes with Lima through railroads, chiefly to reach the mining center of La Oroya. Thousands of Chinese and Chilean immigrants, along with local workers, constructed the initial sections of the railway, at a high cost in terms of human lives. From 1870 to 1872, numerous sick laborers arrived at Lima’s hospitals having become ill while working in the area. They had been exposed to Lutzomyia verrucarum carrying the bacterium Bartonella bacilliformis. These sandflies pass the bacterium into humans’ circulatory systems during noon hours due to their vulnerability to cold temperatures. It causes an initial acute phase of anemia called “Oroya fever,” followed by a chronic dermic infection for which the disease received its name, warts or verrugas. Because the region lacked significant pastoral farming, the increased human activity was optimal to sustain a larger population of these bloodsucking insects. Consequently, temporal alterations in the local ecology exhibited the actions of unacknowledged microscopic actors, impeding the objectives of Peru’s upper class.

Photographs of the upper Rimac valley in Huarochirí province, 1898.
Photographs of the upper Rimac valley in Huarochirí province, 1898.
Photographs by Georges Carré et C. Naud, Éditeurs.
Originally published in Ernesto Odriozola, La Maladie de Carrion, ou la Verruga péruvienne (Paris: G. Carré et C. Naud, 1898). Courtesy of Archive.org.
 This work is licensed under a Creative Commons Public Domain Mark 1.0 License.
This work is licensed under a Creative Commons Public Domain Mark 1.0 License.
It took a little while to discover new aspects of the disease. French-trained Peruvian physician Ernesto Odriozola—greatly benefiting from Daniel Alcides Carrión’s martyrdom in 1885 by inoculating himself with infected blood—presented his findings in a monograph printed in Paris, titled “La Maladie de Carrion.” There he summarized how verrugas was also found in the northern part of the country. This had become noticeable as the massive displacement of Andean seasonal laborers to work in the coastal sugar and cotton estates and the silver-mining centers exposed them areas where the Lutzomyia sandflies were endemic.
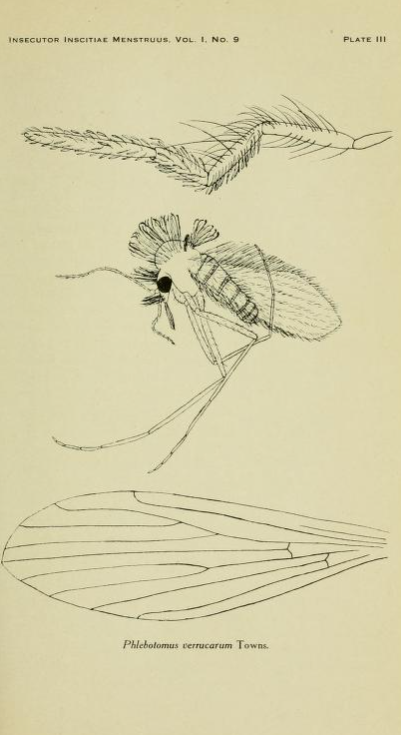
The first illustration of the sandfly Lutzomyia verrucarum, “Preliminary Characterization of the Vector of Verruga, Phlebotomus Verrucarum Sp. Nov.” (1913).
The first illustration of the sandfly Lutzomyia verrucarum, “Preliminary Characterization of the Vector of Verruga, Phlebotomus Verrucarum Sp. Nov.” (1913).
Originally published in Charles H. T. Townsend, “Preliminary Characterization of the Vector of Verruga, Phlebotomus Verrugarum Sp. Nov,” Insecutor Inscitiae Menstruus: A Monthly Journal of Entomology 1, no. 9 (September 1913).
 This work is licensed under a Creative Commons Public Domain Mark 1.0 License.
This work is licensed under a Creative Commons Public Domain Mark 1.0 License.
Odriozola’s example motivated Peruvian physicians to gain international recognition by studying a unique “national” pathology that intrigued the global scientific community. In 1909, Alberto Barton’s discovery of the etiologic agent causing Carrión’s disease showcased the production of biomedical knowledge in a “peripheral” scientific setting. However, mistrust among the emerging group of bacteriologists meant his findings were not widely accepted. In the golden age of tropical medicine, however, other scientists were enthusiastic about unraveling the secrets of the “Peruvian” malady. Some were successful in identifying the transmission vector, shedding light upon the ecological factors of pathogen dissemination. In 1913, American entomologist Charles Townsend captured and described eight specimens of the Phlebotomus sandfly in Huarochirí, finally allowing the flag-bearer of Peru’s medical pride to be visualized (see illustration below). Even with partial support from the Peruvian medical community, skepticism persisted among physicians until Hideyo Noguchi, a Japanese doctor who worked at the Rockefeller Institute in New York, confirmed Barton’s and Townsend’s findings in the late 1920s.
Due to limited resources for laboratory-based research, applied science gained prominence in Peru’s biomedical activities. The book Estudios sobre geografía médica by Sebastian Lorente Patrón and Raul Flores was a significant product of this shift. Published in 1925 under Augusto B. Leguía’s dictatorship, it provided a complete mapping of infectious diseases in the country, enabling Peruvian physicians to produce a national disease ecology. By dividing the territory into different colored areas (as seen in figure 4), these maps became symbols of the physicians’ power and the government’s effort to understand the relationship between the environment and human health.
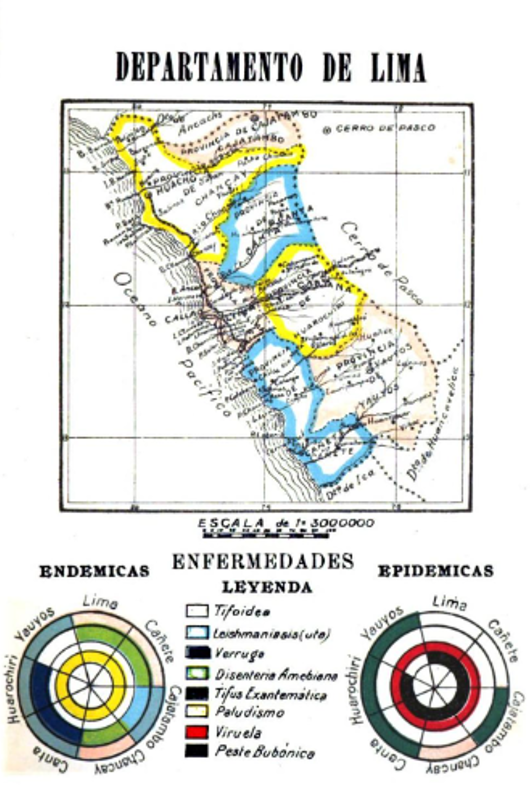
Map of the main pathologies of the Department of Lima, 1925.
Map of the main pathologies of the Department of Lima, 1925.
Originally published in Sebastián Lorente and Raul Flores, Estudios sobre geografía médica y patología del Perú. Lima: Imprenta Americana, 1925.
 This work is licensed under a Creative Commons Public Domain Mark 1.0 License.
This work is licensed under a Creative Commons Public Domain Mark 1.0 License.
With better understanding of the transmission and distribution of Carrión’s disease, past Peruvian scientific achievements were now recognized by important institutions in the medical arena. In 1937, Richard Strong, leader of the first Harvard Expedition to Peru in 1913, confirmed Barton’s findings by naming the bacteria’s genus after him (Bartonella). By acknowledging that both Oroya fever and verrugas had the same etiological agent, Strong made Barton’s achievements widely known, compensating for having argued that the Peruvian physician was mistaken more than two decades earlier.
For the bloodsucking insects themselves, however, a renowned status among the main sites of medical knowledge didn’t come as good news. The discovery of pesticidal properties in organochlorine compounds, such as DDT, laid the ground for their largescale use by US forces in the Mediterranean and South Pacific to protect troops against malaria, typhoid fever, and dysentery. Under the guise of the Pan American Health Organization, Peru, along with other countries in the region that had recently discovered Carrión’s disease in their territory, followed a postwar regime of disease eradication using organopesticides. However, with the later decline of cooperative assistance from multilateral organisms, and the lack of domestic support for consistent scientific research, the disease became neglected on the global health agenda. Nowadays, with at least four species of the Lutzomyia genus carrying the B. bacilliformis, these insects are still present in the poorest regions of these Andean countries, although they no longer hold the status they once enjoyed in the scientific community—which now is only commemorated in history books and by the busts of the scientists who studied them.
How to cite
Mogrovejo, José Ignacio. “A More-than-Human Viewpoint on the History of a ‘Peruvian’ Disease.” Environment & Society Portal, Arcadia (Autumn 2023), no. 20. Rachel Carson Center for Environment and Society. doi:10.5282/rcc/9692.
ISSN 2199-3408
Environment & Society Portal, Arcadia
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
2023 José Ignacio Mogrovejo
This refers only to the text and does not include any image rights.
Please click on an image to view its individual rights status.
- Cueto, Marcos. “Tropical Medicine and Bacteriology in Boston and Peru: Studies of Carrión’s Disease in the Early Twentieth Century.” Medical History 40, no. 3 (1996): 344–64.
- Cueto, Marcos. “Nationalism, Carrión’s Disease and Medical Geography in the Peruvian Andes.” History and Philosophy of the Life Sciences 25, no. 3 (2003): 319–35.
- Gomes, Cláudia, and Joaquim Ruiz. “Carrion’s Disease: The Sound of Silence.” Clinical Microbiology Reviews 31, no. 1 (2018). doi:10.1128/cmr.00056-17.
- Lorente, Sebastián, and Raul Flores. Estudios sobre geografía médica y patología del Perú. Lima: Imprenta Americana, 1925.
- Odriozola, Ernesto. La Maladie de Carrion, ou la Verruga péruvienne. Paris: G. Carré et C. Naud, 1898.
- O’Gorman, Emily, and Andrea Gaynor. “More-than-Human Histories.” Environmental History 25, no. 4 (2020): 711–35.
- Townsend, Charles. “Preliminary Characterization of the Vector of Verruga, Phlebotomus Verrucarum Sp. Nov.” Insecutor Inscitiae Menstruus 1, no. 9 (1913): 107–9.